Can Inhaling Gluten Trigger Symptoms in Sensitive Individuals?
An astonishing number of people following a strict gluten-free diet and lifestyle remain symptomatic.
If they are very compliant with gluten elimination but still experience negative symptoms associated with gluten, could something else be a trigger?
Lab tests, like the Vibrant Wheat Zoomer, can provide that insight.
On a daily basis, Vibrant’s clinical team consults with gluten-free patients who have completed Vibrant’s Wheat Zoomer test.
The beauty of Vibrant’s Wheat Zoomer is in identifying wheat and gluten-related disorders and also assessing one’s level of exposure to wheat and gluten.
Surprisingly, many strictly gluten-free individuals find their lab results come back indicating high levels of antibodies to wheat and/or gluten.
Why is this?
Let’s Start With Going on a Gluten-free Diet
When one initially learns that they need to avoid gluten, the first step is to remove the obvious sources.
The average person knows that items such as bread and pasta will need to be avoided, but what's next? Numerous educational resources can provide that education, including but not limited to clinicians, blogs, and books.
Reading product labels that advertise their products as gluten-free is also an obvious means to find gluten-free products. It's important to note that foods labeled gluten-free contain less than 20 ppm (parts per million), and, therefore, are not necessarily zero percent gluten.
Going gluten-free can be an overwhelming process. Generally speaking, once the major sources of gluten are removed from the diet, it is imperative to read labels on all packaged foods and then move on to toiletries and cosmetics.
Those avoiding gluten need to use gluten-free lip balm, toothpaste, chewing gum, medications, supplements, and sunscreen, to name a few items that do not generally cross the mind when starting this journey.
Is that everything?
Ideally, patients should feel better at this point. They should find that their health has improved, maybe symptoms they didn't even realize you were experiencing are no longer present, and their overall well-being has improved.
Sounds great, right?
But what if they still feel like something is still off? You can run a test to assess their gluten-free compliance efforts.
Case Study #1: 13-year-old girl on a strict gluten-free diet
The Vibrant clinical team has encountered numerous patients who receive lab results and claim they must be incorrect.
Why? Because their results indicate exposure has occurred with non-gluten proteins of wheat and/or gluten proteins when they claim to be strict gluten-free dieters.
During a consultation with Vibrant’s clinical team, a lengthy list of possible unrealized exposures is reviewed:
- “Do you lick the glue on envelopes or stamps?”
- “Do you eat any meals outside of your home?”
- “Do you know how to properly read labels?”
- “Do you know that even gluten-free packaged foods can contain minimal ppm of gluten?”
- “Do you take medications or supplements that contain gluten?” And so on…
Recently, we've come across patients who seem so educated and so compliant that even we were scratching our heads. Then, we started exploring inhalation.
Do you know that all forms of exposure to wheat and gluten need to be considered?
Below are the results of a 13-year-old female that developed orthorexia, an eating disorder developed in pursuit of a healthy diet, because she was fearful and anxious about not feeling well whenever she ate.
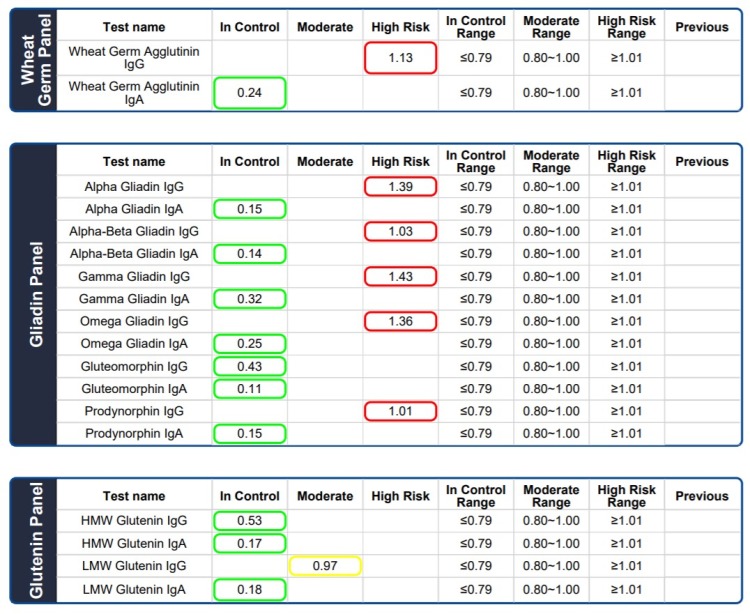
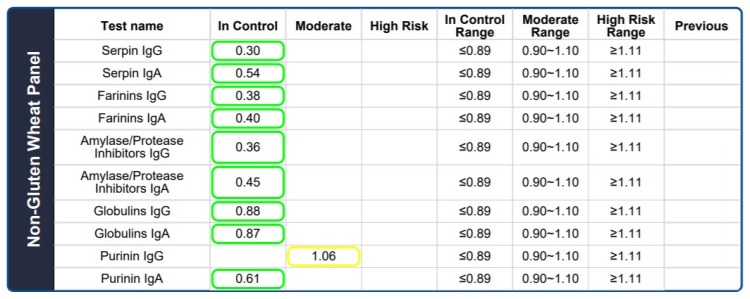
The child's eating habits are strict. The mother stated that she knows that the child does not cheat due to her fear of becoming sick from eating.
Are you curious what the source of non-gluten wheat proteins and gluten proteins for this strict teenager is? The answer is wheat farms. This family lives in a farming community that farms wheat and thus, they are surrounded by wheat, and its residual wheat dust, all around their home.
Case Study #2: 73-year-old female on a long-term gluten-free diet
Another interesting case study is a 73-year-old female who has been gluten-free for decades, does not consume processed foods, and even makes most of her own toiletries and beauty products.
She also showed elevated antibodies that are indicative of exposure to non-gluten proteins of wheat, as well as gluten-containing proteins on her Vibrant Wheat Zoomer lab results.
While discussing the previous story about the young, compliant, now orthorexic girl, it was discovered that this patient also lives within 10 miles of wheat farms. It's possible that she is also at risk for wheat inhalation.
Case Study #3: A baking instructor on a gluten-free diet
Clinical team members have shared a similar story about a clinical consultation with a patient that is extremely careful not to eat or handle gluten; yet, the patient obtained lab results indicating that she was exposed to and reacting to gluten.
The patient is a baker who teaches baking classes that include wheat products. She wears gloves and does not consume wheat. In this third scenario, the patient is inhaling the wheat flour that is dispersed in the air during the process of preparing the baked goods.
Why does inhaling wheat trigger symptoms?
When we inhale wheat, which includes both non-gluten and gluten-containing proteins in wheat, those particles become trapped in our saliva and nasal passages, entering into mucous membranes and further traveling into our intestinal tract.
Numerous studies show that inhaling gluten can trigger symptoms of celiac disease, gluten sensitivity, wheat allergies, and asthma in sensitive individuals.1,2
How to Avoid Inhaling Gluten
First, individuals need to know where gluten inhalation may occur so they can take precautions to avoid inhaling the particles:
Never use gluten-containing flour or visit bakeries, pizzerias, or homes where gluten-containing flour is used.
If you must be around a bakery that uses gluten-containing flour, such as the grocery store, or a pizzeria, exercise caution. Some bakers say that it can take 36-48 hours for flour to settle from the air—that's up to 2 days!
Avoid construction sites, especially during drywall work, and avoid ready-made spackling, as most contain wheat.
These are an often-overlooked source of hidden gluten exposure.
Consider using a face mask in certain situations.
You can find a full respiratory mask for about $40 in home improvement stores. If you have any respiratory conditions, use a respiratory mask with caution.
Switch to gluten-free pet food.
Even if someone else feeds your pet or moves the bowl to a place you do not go, it would be much easier to switch your pet to gluten-free food.
If your patient has persistent symptoms despite adhering to a strict gluten-free diet, consider a Vibrant Wheat Zoomer test to assess their antibodies to all the possible proteins in wheat and gluten. With 100% accuracy, this test can reveal if they have been successfully avoiding gluten and/or wheat.
Suzette Garcia, MSc: MHNE, is a Clinical Educator at Vibrant Wellness. She is a Board Certified Holistic Nutritionist® certified through the Holistic Nutrition Credentialing Board (HNCB) and a Professional Member of the National Association of Nutrition Professionals (NANP). Suzette obtained her Master of Science in Health and Nutrition Education (MHNE) from Hawthorn University and has spent her nutrition career working in the field of functional health and nutrition with a strong focus on food sensitivities, gut health, and hormones. Suzette is fluent in both English and Spanish and offers interpretation of lab test results in both languages.
In her spare time, you can find Suzette spending most of her time on the waters of South Florida, vacationing to tropical locations, practicing and teaching yoga, working on home improvements, eating good food, and furthering her education in the field of functional health and nutrition. She is a native Floridian.
References
- Khan et al (2018). Immunological study of different fraction of wheat proteins. Pak J Pharm Sci. 2018 Jul;31(4):1437-1440. https://www.ncbi.nlm.nih.gov/pubmed/30033431
- Khodadadi et al (2011). Exposure to respirable flour dust and gliadin in wheat flour mills. J Occup Health. 2011;53(6):417-22. Epub 2011 Oct 13. https://www.ncbi.nlm.nih.gov/pubmed/21996928
 By
By



