The Gut Barrier's Role in Micronutrient Absorption
It’s well known that the foods we eat have a tremendous influence on our overall well-being and ability to thrive. However, their benefits can only be fully realized when our digestive system functions optimally.
Beyond the quality of the food we consume, the health of our gut and its intricate mechanisms is equally crucial.
At the core of gut health lies the gut or intestinal barrier. This fundamental system ensures efficient nutrient absorption and shields our body from potential harm.
When this barrier is compromised, it can cause conditions like increased intestinal permeability (leaky gut), nutrient malabsorption, and chronic illness.
In this article, we'll delve into the complexities of the gut barrier, exploring its vital role in micronutrient absorption. We'll also examine the relationship between malabsorption and leaky gut. Plus, you’ll learn precision testing options to promote healing and restore digestive balance.
Understanding the Gut Barrier
Proper functioning of the gut is central to our health. This organ system begins in the mouth and runs down to the rectum, and it’s responsible for digestion, nutrient absorption, and elimination of waste.
But the role of the gut isn't limited to digestive functions—it makes up 70–80% of our immune system cells and has a huge influence on the rest of the body.
One foundational component of the gut and gastrointestinal tract is the gut barrier.
This barrier is made up of surface mucus, an epithelial layer of cells, and immune defenses. It separates the internal environment of our gut from the rest of the body.
You can think of the gut barrier as a security checkpoint. Its job is to allow beneficial substances like micronutrients into the body, and prevent harmful substances like toxins and bacteria from entering.
When the intestinal barrier is compromised, you’ll begin to see conditions like leaky gut, also known as increased intestinal permeability.
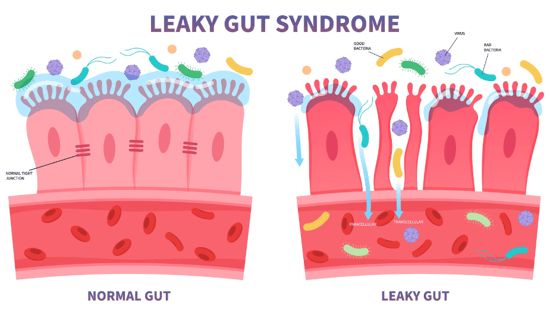
Leaky gut occurs when there are gaps or loosened tight junctions in the intestinal cells of the gut barrier. This allows harmful substances like bacteria and food antigens to ‘leak’ through and circulate the body.
The gut influences virtually every part of the body. Thus, intestinal permeability is linked to both gastrointestinal diseases (GI) like celiac and irritable bowel syndrome (IBS), and conditions in other body systems like Alzheimer's, Parkinson's, and diabetes.
Intestinal permeability is harmful largely due to its accompanying counterpart—malabsorption.
But before dissecting malabsorption, let’s look at how nutrients get absorbed when the gut is functioning properly.
Nutrient Absorption
Nutrient absorption occurs mainly in the small intestine and is regulated by the gut barrier.
The gut barrier is composed of a single layer of epithelial cells, tight junctions, and a mucous layer. The tight junction proteins hold the layer of epithelial cells together, while the layer of mucous lies on the surface.
This mucous layer is vital in preventing bacteria and pathogens from getting into the body.
To absorb nutrients efficiently, the small intestine requires a large surface area—estimated to be 30m2 or 323 square feet. A large part of this surface area comes from the villi and microvilli that line intestinal cells.
Villi are tiny, finger-like structures found on the layer of epithelial cells. Microvilli are even tinier, hair-like structures you'd find on the surface of individual cells that comprise the villi. Thousands of microvilli can cover the surface of each cell.
The body utilizes various modes of transport to help nutrients pass the gut barrier and get absorbed into the bloodstream.
These include:
- Active transport
- Passive diffusion
- Facilitated diffusion
- Endocytosis
- Emulsification
Nutrients also get help from transport proteins to travel safely across the gut barrier into the rest of the body.
Lastly, the intestinal barrier is a semi-permeable membrane. This means certain particles can pass through while others can’t. This allows beneficial substances like nutrients to pass through while preventing harmful antigens and pathogens from entering.
Micronutrients

One of the main roles of the gut barrier is to facilitate the absorption of micronutrients. Micronutrients are vitamins and minerals that are vital for proper functioning of the body. The body only requires these nutrients in small amounts, but they have a significant impact on health.
Micronutrients carry out a range of functions, including helping the body produce enzymes, hormones, and other products necessary for normal growth and development.
They also play a key role in homeostasis of the digestive system.
Nutrients like vitamin A and D support the integrity of the epithelial barrier, the innate and adaptive immune system, and gut microbiota.
Vitamin A or D deficiency reduces microbial diversity in the gut.
Further, vitamin A and D help support intestinal barrier function by regulating the expression of tight junction molecules.
Another critical micronutrient is the amino acid glutamine—the most important fuel for enterocytes and immune cells. Enterocytes are specialized cells that support nutrient absorption.
Deficiency in any of the micronutrients can cause severe and even life-threatening conditions.
Symptoms of micronutrient deficiency include:
- Stress
- Fatigue
- Depression or anxiety
- Skin problems
- Numbness or tingling in extremities
- Weakened immune system
- Lack of concentration/Brain fog
- Fluctuating weight
- Neurological symptoms (impaired memory, confusion, ataxia, loss of balance, tremors)
- Stubborn weight gain
- Sudden, unexplained weight loss
- Digestive abnormalities: diarrhea, constipation, excessive bloating
To prevent damage to the body, it is essential to address the source of micronutrient deficiencies. One potential source? Malabsorption.
Malabsorption
If your patients are consuming nutrient-dense diets but still experiencing nutrient deficiencies, malabsorption may be the culprit.
The health of intestinal cells, and the protective mucous coating above them, directly impacts how efficiently we digest and absorb nutrients from food and supplements.
Intestinal permeability and malabsorption often accompany each other due to inflamed intestinal epithelial cells.
If epithelial cells are inflamed, there's a loss of surface area in the small intestine, contributing to malabsorption.
Depending on the location of the inflammation or cellular damage, which nutrients aren't being absorbed properly can vary.
Factors like diet, cytokines, and disease can impact the intestinal barrier and cause malabsorption.
Many diseases are associated with impaired gut barrier function including inflammatory bowel disease and autoimmune conditions like celiac.
Whether diseases are causing gut dysfunction and malabsorption —or vice versa — is controversial. A dysfunctional barrier and gastrointestinal disease can act as the cause and effect of one another, creating a vicious cycle of chronic inflammation.
Gut Health Testing
The best way to gain an intricate view of intestinal permeability and inflammation is through gut health testing.

The Vibrant Wellness Gut Zoomer assesses:
- Over 170 species of bacteria
- 67 pathogenic microorganisms
- Functional markers of digestion and inflammation
- The entirety of genetic information (DNA) from all microorganisms tested
This test measures hundreds of species of microbes at once, giving you detailed information on intestinal permeability, gut microbiota levels, and inflammation.
The Gut Zoomer will help you determine if intestinal permeability, dysbiosis, and malabsorption are at the root of your patients’ nutrient deficiencies.
Micronutrients Testing

To determine if your patients have healthy levels of nutrients, you can use precision testing like the Micronutrients Panel.
This test will help you accurately assess your patients’ micronutrient levels.
When addressing nutrient deficiencies, it’s critical to remember that all micronutrients exist in a delicate balance inside the body.
Thus, hyper-dosing with many individual micronutrients can potentially cause harm.
Insights from the Micronutrients panel will help you pinpoint which nutrients aren't being absorbed properly, enabling personalized treatment plans to address specific needs.
The Micronutrients test detects direct levels of extra- and intracellular micronutrients by analyzing absorption at the gastrointestinal barrier and cellular membrane, so you can objectively determine root causes of malnutrition and inflammation.
The panel detects precise levels of:
- Vitamins
- Minerals
- Co-factors
- Amino acids
- Metabolites
- Antioxidants
- And essential fatty acids
Coupling the Gut Zoomer with the Micronutrients test will help determine if leaky gut, malabsorption, or digestive disorders are contributing to your patients’ nutrient deficiencies.
Gut function and nutrient absorption influence one another and are both crucial mechanisms for gastrointestinal and general health.
The gut barrier is designed to regulate the constant stream of nutrients, pathogens, and substances that enter the body. When this barrier gets damaged, it can lead to intestinal permeability, malabsorption, and chronic illness, resulting in a vicious cycle.
With precision testing like the Gut Zoomer and Micronutrients panel, you can gain a holistic understanding of the relationship between these mechanisms. This allows you to create personalized solutions to address nutrient deficiencies and inflammation and promote healing.
Regulatory Statement:
The general wellness test intended uses relate to sustaining or offering general improvement to functions associated with a general state of health while making reference to diseases or conditions. This test has been laboratory developed and its performance characteristics determined by Vibrant America LLC and Vibrant Genomics, a CLIA-certified and CAP-accredited laboratory performing the test. The lab tests referenced have not been cleared or approved by the U.S. Food and Drug Administration (FDA). Although FDA does not currently clear or approve laboratory-developed tests in the U.S., certification of the laboratory is required under CLIA to ensure the quality and validity of the test
 By
By



